Understanding Family Accommodation in OCD: When Helping Makes It Worse
I’m just going to come out and say it: OCD (obsessive-compulsive disorder) is a sneaky little bugger.
I’m a therapist in North Vancouver (British Columbia, Canada) and I specialize in working with anxiety and OCD in teens and young adults. One of the most important pieces of my work is looking at family accommodation.
But before we get into that, I need to highlight some really important information:
The person with OCD (aka your loved one) should be involved at every step mentioned in this post. Consent and collaboration are SO important, both for recovery and maintaining your relationship with them.
Changing how we help is incredibly hard for everyone, especially the person with OCD. It can feel cold and cruel (all the more reason why their buy-in is essential).
Support from a professional (like a therapist) is highly recommended.
So, what in the world is family accommodation?
I’m so glad you asked!
Family accommodation is when the people in your circle of support (family, friends, teachers, coaches, etc.) do things to help and support you that are unknowingly contributing to and worsening your OCD.
OCD is sneaky and has a wonderful way of convincing us that something is helping, when really, it’s keeping the OCD going STRONG. OCD is good at getting what it needs to grow and get stronger. It knows how to tap into the support of our loved ones for its benefit.
Our support circles are doing the best that they can. They truly believe they’re helping because the things they do show that they know you, they care about you, and they’re thinking of you.
For example, if someone has a fear that they will panic and not be able to escape if they don’t have an aisle seat at a sporting event, their family/friend might go out of their way to find and purchase an aisle seat. “I remembered that you don’t like to feel trapped so I got us aisle seats!”
Little things like this show that we matter to the people in our lives - they see and accept us for who we are, OCD fears and all. And that is a beautiful thing.
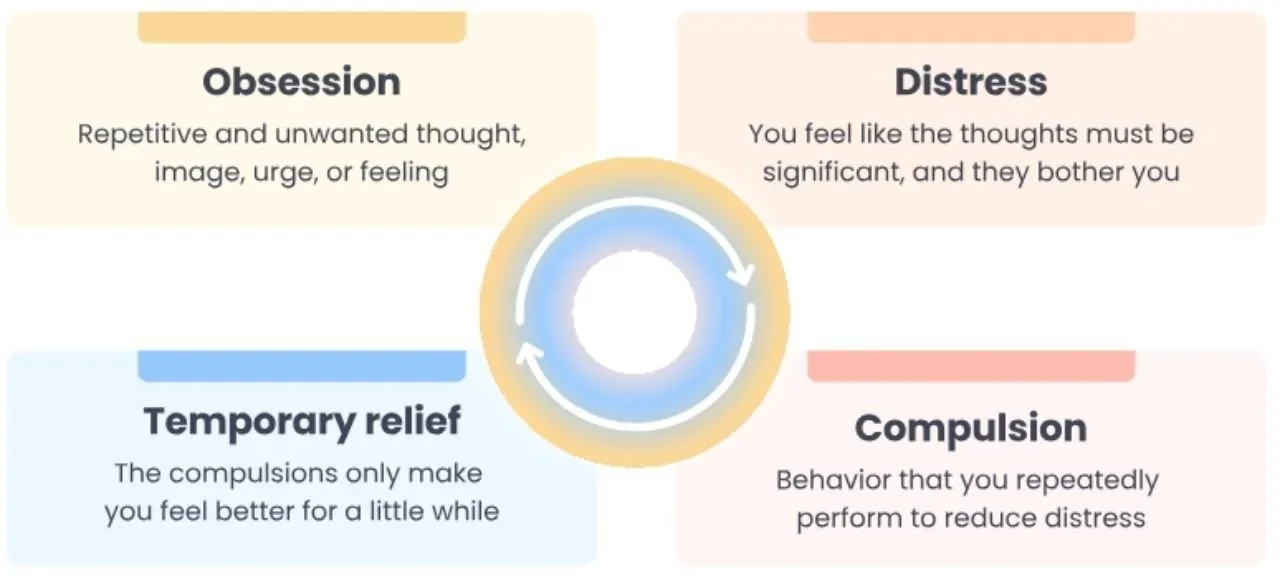
To help us understand how helping can feed OCD, we need to first look at the OCD cycle.
Image taken from NOCD.
The cycle works like this:
Intrusive thought. People with OCD will first experience an intrusive/distressing/unwanted/anxious thought. This can be something like: Is my headache brain cancer?, what if I accidentally plagiarized my assignment? or an intrusive, disturbing image like hurting someone.
Assigning meaning. Following the intrusive thought/image, our brains usually attach some kind of meaning to the thought. For example, if you have a thought about accidentally plagiarizing, you might believe that this means you’re irresponsible because you should have double checked.
Anxiety/fear/discomfort rises. This is where OCD does a wonderful job of pulling us into spirals.
What if I really did accidentally plagiarize? My teacher won’t believe it was an accident.
How could I let this happen?
What if I get expelled? My career could be over before I’m done school.
What if this ruins my life?
Compulsion(s). With our anxiety high, it’s only natural to want to do something to decrease it and get some relief. Our example student might decide to:
Run their assignment through a plagiarism detector even though it has already been submitted to confirm that they didn’t accidentally plagiarize.
Email their teacher to let them know that they believe they didn’t properly rephrase something and may have accidentally plagiarized.
Repeat a prayer, phrase, or mantra in an effort to feel more in control, reduce uncertainty, and try to prevent a feared situation from happening or make sure things turn out okay.
Ask someone from their support circle if they believe someone could accidentally plagiarize.
Temporary relief. The goal of compulsions is to provide relief to the distress, anxiety, and discomfort caused by the initial thought and the spiral. But that relief is temporary. This is really important!
Negative reinforcement. When doing the compulsion results in a decrease in discomfort/distress/anxiety, our brain learns that when the scary thought happens, the best way to relieve ourselves from these hard emotions is to do the compulsions. Each time we complete this cycle, OCD gets stronger. I like to to think of this like taking a pill for a headache - if the headache goes away each time we take the pill, the behaviour of taking the pill gets reinforced, so next time we have a headache, we might be more likely to reach for that pill.
Where does family accommodation typically occur?
Supporters can do or say something that inadvertently strengthens the cycle at any point of the cycle.
Intrusive thought & assigning meaning
The most common mistake I see here is when supporters either agree or challenge the intrusive thought and the meaning surrounding it. Let’s look at some examples, using our sample intrusive thought of what if I accidentally plagiarized.
Agreeing/supporting the thought
You might be inclined to validate your loved one by sharing support for their feared thought. This happens most commonly when the person with OCD is worried that their thought is irrational and they’re “spiraling for no reason.” Naturally, we want to reassure them that they aren’t being irrational - that their fear is “totally normal.”
Unfortunately, when we do this, we reinforce the fear that their intrusive thought could actually be real or could actually happen.
When we say “no, that’s not crazy at all! Actually, my cousin was accused of plagiarizing last year so it does happen.”
OCD might hear “This is real and likely, so we should sound the anxiety alarm and deal with it urgently.”
We think we’re communicating that it’s okay, it’s a valid fear, weird things happen sometimes. and everything turns out fine. But the message can be received as: your biggest fear is going to happen.
Disagree/challenging the thought
Another common inclination is to present evidence that either disproves the feared outcome, or decreases its likelihood. When this happens, it often comes from a kind place of wanting to provide reassurance that the feared outcome isn’t going to happen.
This can look like: “Professors only really care if you copy and pasted. Unless you did that, it’s pretty much impossible to be accused of plagiarism.”
There are a few reasons why responses like this can make OCD stronger:
OCD feeds on doubt. It doesn’t matter how unlikely something is, OCD cares that it’s technically POSSIBLE.
OCD has an comeback for everything. You say that they would need to literally copy and paste for it to be plagiarism, OCD asks: “could I have copy and pasted into my assignment, hoping to come back later to rephrase it, but I forgot and submitted the assignment as is?”
Checking for evidence can become a compulsion. Next time an intrusive thought comes up, OCD asks us to search for any evidence against it.
Dismissing the thought
Much less common, but sometimes we might tell someone “don’t worry about that” when they share an OCD-related thought. While we mean well, this might signal to them that you are not a trusted source of support.
Compulsions
Another common part of the cycle where supporters tend to accidentally feed OCD is with compulsions. This one is SO COMMON.
Providing reassurance
One sneaky OCD compulsions is reassurance seeking - looking for confirmation that everything is okay. This can look like:
“Do you think I could have accidentally plagiarized?”
“Could you check this reference and tell me whether it could be plagiarism?”
“Do you think I’ll get expelled?”
“Has this ever happened to you?”
These questions seem harmless, but answering them teaches OCD that the thought was important and urgent, and that we need to have these questions answered to before we can move forward. As time goes on, compulsions can become more demanding, seeking more and more reassurance before feeling satisfied.
Participating in compulsions and/or safety behaviours
Supporters who participate in compulsions, safety behaviours, or rituals usually do it because they believe they are showing their loved one that they are not too much. Family will often tell me, “I wanted them to see that I was okay to be right there with them,” or “I just wanted them to feel better and [doing the compulsion] made the anxiety go away.” But remember: compulsions/rituals/safety behaviours only decrease the anxiety temporarily. In the long run, they actually communicate to the brain that the though is dangerous, urgent, and must be responded to immediately, making the OCD louder and stronger.
Here are some examples of how a supporter might participate in a compulsion:
Adhering to strict rituals our routines (walking/driving the same route to the store, praying in the same order before bed, unplugging electronics before leaving home, touching certain objects when passing them, disinfecting items when they come into the house)
Engaging in checking behaviours (making sure the stove and other household items are off before leaving the house, excessively checking pets or each other for “lumps,” excessively checking flight confirmation to make sure you remember the date/time correctly)
Reassurance seeking (Googling questions, reviewing assignments before they submit)
While supporters might not directly involve themselves in compulsions, they may indirectly participate by allowing the time and space their loved one needs to complete their compulsions. Supporters who participate this way might create a time buffer when making plans in case their loved one’s compulsions take extra time.
Okay, so what do you do instead?
Great question! I’m so glad you asked.
This is where you might want to take some notes. But don’t worry, it’s not nearly as complicated as calculus (I actually loved calculus, but I digress..).
Sit with them in the discomfort
The thoughts/images/sensations your loved one experiences often cause significant distress, anxiety, and discomfort. One way to join them, validate them, and show them that they are not “too much” is to sit with them in that discomfort. Put down what you’re doing and give them your undivided attention - not to try and “fix” their discomfort, not to tell them that everything is going to be okay, and not to challenge their fear. Sit with them in the discomfort of experiencing their intense distress without doing anything to eliminate the distress.
Here are some things you can say:
“I see how [distressed/anxious/etc.] this is making you. I know this must be really hard for you. Let’s sit together in the uncertainty.”
“I know you’re working really hard not to do your compulsion right now. Let’s keep holding off together.”
“You don’t know if [feared event/thought] is true and the uncertainty is very scary.”
“OCD wants you to [compulsion], but you want to [their reason to push through recovery - values, goals, etc.]. Let’s move towards that together by just sitting with this uncertainty a little longer.”
“I know you want [reassurance/participating in a ritual/etc.] right now. While I can’t do that, I can sit with you through the distress of not completing your compulsion.”
Note: avoid saying things like “it’s just OCD,” or “you can do this,” or “everything is fine/you’re safe,” as these are all different ways that we provide reassurance.
Disengage from your involvement in compulsions/rituals and safety behaviours
This might be the most challenging change for supporters. Your loved one has likely come to expect your participation; in fact, your participation might be integral to the compulsion at this point (oops!). To your loved one, withdrawing from involvement can leave them feeling isolated, ashamed, and unsupported, especially when distress is peaked and relief (via compulsions) is prevented.
Here are some things you can say:
“I wanted to let you know that I’m no longer able to [go home to check the stove during my workday, book aisle seats, scrub the groceries before putting them away, etc.]. I really care about you and I know that my involvement in your [compulsions/rituals/safety behaviours] is making your OCD stronger. I’m here to support you in other ways.”
“I need to set a boundary around [compulsions/rituals/safety behaviours].”
Discourage any talk about the thought
Why, you might ask? It’s very easy for the conversation to turn into something else, like: reassurance seeking, challenging the thought, confessing (this is a type of compulsion), trying to “figure out” the thought. It’s a slippery slope. With OCD, we don’t want to give the thought any of our voluntary attention.
Here are some things you can say:
“You can certainly share your thought if it helps, but I won’t be responding to it.”
“Thank you for sharing. I can tell that you’re experiencing a lot of distress right now.”
“Now that it’s out in the open, let’s not give it any additional attention.”
What if I make a mistake?
Instead of “what if I make a mistake,” I frame it like this: “when I make a mistake…”
OCD is tricky, compulsions can be sneaky, and at the end of the day, you’re only human. You will probably make a mistake and accidentally accommodate your loved one’s OCD. But that’s not the end of the world.
Here are a few ways to get back on track after accidentally accommodating OCD:
If you provided reassurance, reintroduce some uncertainty: “But I could be wrong.”
If you are participating in a compulsion, name it, and disengage: “Ooops, I noticed I just double-checked the stove. I’m not going to be checking again.”
If you are participating in avoidance, name it, and face it (if you can): “I just realized I took a detour away from the cemetery… I think we should go back and drive by it.”
At the end of the day, remember that this is a collaboration for the benefit of your loved one.
This is for them. They need to be on board. You are a team, tackling this challenging work together. A united front.
With your loving support, they will get through the difficult work of OCD recovery.
Need some help along the way? I offer a free 15-20 minute consultation to see if we’re a good fit.